Understanding Cognitive Behavioural Therapy (CBT): How Thoughts, Feelings, and Behaviours Connect
Cognitive Behavioural Therapy (CBT) is one of the most widely used and researched forms of psychotherapy today. You may have heard the term before, but aren’t exactly sure what it actually involves. In simple terms, CBT focuses on understanding how our thoughts influence our emotions and behaviours. When we learn to notice and challenge unhelpful thinking patterns, it can lead to meaningful changes in how we feel and how we act.
This blog explores what CBT is, how it works, what a typical session might look like, who it can help, and why it is considered an evidence-based approach to mental health care.
What Is Cognitive Behavioural Therapy?
Cognitive Behavioural Therapy is a structured, goal-oriented form of psychotherapy that focuses on the connection between thoughts, emotions, and behaviours. The core idea behind CBT is that the way we interpret situations affects how we feel and how we respond. For example, two people might experience the same event but interpret it very differently. One person might see it as a failure, while another sees it as a learning opportunity. Those different interpretations can lead to very different emotional reactions and behaviours. CBT works by helping individuals identify patterns of thinking that may be unhelpful or inaccurate and gradually replace them with more balanced, realistic perspectives. Over time, this shift in thinking can lead to improvements in mood, behaviour, and overall wellbeing.
How CBT Works: The Cognitive Model
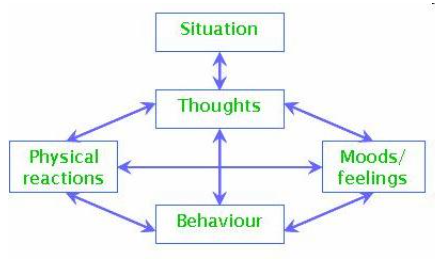
At the heart of CBT is the idea that meaning matters. It’s not simply what happens to us that shapes our emotional response, but how we interpret or make sense of the experience. CBT looks at three interconnected parts of our internal experience:
Thoughts
These include the quick, automatic thoughts that pass through our minds throughout the day. These thoughts often happen so quickly that we don’t even notice them, but they can strongly influence our emotions.
Emotions
How we feel emotionally, such as anxiety, sadness, frustration, or shame.
Behaviours
The actions we take in response to our thoughts and emotions, such as avoiding situations, withdrawing from others, or engaging in helpful coping strategies.
CBT often begins by helping people notice their automatic thoughts, which are the immediate interpretations that pop up in response to situations. These thoughts are usually brief, spontaneous, and often accepted as true without much reflection. Once identified, the therapist and client work together to evaluate whether those thoughts are accurate or helpful. Over time, therapy may also explore deeper thinking patterns, such as underlying assumptions and core beliefs that shape how a person sees themselves, others, and the world.
Diagram of the Cognitive Model
What Happens in a CBT Session?
CBT sessions tend to be collaborative and structured. Rather than the therapist simply interpreting the client’s experiences, both the therapist and client work together to explore thoughts, behaviours, and patterns that may be contributing to distress.
A typical CBT session might include:
Reviewing current challenges
The client may discuss recent experiences, emotional reactions, or difficult situations that occurred since the last session.
Identifying patterns in thoughts and behaviours
The therapist helps the client notice automatic thoughts or behavioural patterns that may be influencing their emotional experience.
Exploring alternative perspectives
Together, the therapist and client examine whether certain thoughts are realistic, helpful, or overly critical.
Developing practical strategies
CBT often includes skill-building exercises, coping strategies, or behavioural experiments that clients can try between sessions.
Setting goals or reflections for the week
Clients may leave with new strategies or reflections to practice in everyday life.
The Role of the Therapeutic Relationship
Although CBT focuses on thoughts and behaviours, the relationship between therapist and client remains essential. Trust, empathy, and collaboration create the foundation that allows meaningful therapeutic work to happen. CBT emphasizes a collaborative alliance, where the therapist brings expertise in psychological strategies and the client brings expertise in their own experiences. Both perspectives are important. Therapists also aim to create a respectful, culturally responsive environment where clients feel comfortable exploring their thoughts, emotions, and personal experiences.
Who Can CBT Help?
Research has shown that CBT can be particularly effective for conditions such as:
Anxiety disorders - Including generalized anxiety, panic disorder, and social anxiety.
Depression - Helping individuals challenge negative thinking patterns and re-engage in meaningful activities.
Obsessive-Compulsive Disorder (OCD) - Often combined with exposure-based strategies to reduce compulsive behaviours.
Stress and life transitions - Supporting individuals in developing healthier coping strategies.
Low self-esteem and perfectionism - Helping people examine underlying beliefs about themselves and their abilities.
Why CBT Is Considered Evidence-Based
CBT is often described as an evidence-based therapy, meaning its effectiveness has been supported by extensive scientific research. Since its development in the 1960s by psychiatrist Dr. Aaron Beck, CBT has been studied in hundreds of clinical trials across many mental health conditions. Researchers have consistently found that CBT can reduce symptoms of anxiety, depression, and other psychological concerns. It is frequently recommended in clinical guidelines because it combines theoretical understanding with measurable outcomes. CBT also tends to include ongoing assessment and feedback, such as questionnaires or self-rating scales that track changes in mood, stress, or symptoms over time. This helps both therapists and clients monitor progress and adjust strategies as needed.
What Makes CBT Different?
One of the distinguishing features of CBT is its active and skill-based approach. Rather than focusing only on insight or reflection, CBT emphasizes learning practical tools that can be applied in everyday situations. These tools may include:
Identifying and challenging unhelpful thoughts
Practicing new behaviours
Developing coping strategies for stress or anxiety
Gradually facing feared situations in manageable steps
Building healthier thinking patterns over time
The goal is not simply to talk about problems, but to develop skills that help individuals navigate challenges more effectively.
Final Thoughts: Learning New Ways of Thinking and Responding
Cognitive Behavioural Therapy offers a practical and empowering way to understand the connection between thoughts, emotions, and behaviours. By learning to recognize and question unhelpful thinking patterns, individuals can develop healthier ways of responding to life’s challenges.
For many people, CBT provides tools that extend far beyond therapy sessions. The skills learned can support resilience, emotional awareness, and long-term mental wellbeing.
While every person’s experience is different, CBT offers a structured and collaborative approach that can help people better understand their minds and create meaningful, lasting change.